A Great Fiducial Marker
Applications in any organ
Safe to use in almost any inner organ
Gold Anchor is safe for use in almost any organ due to its ultra-thin needles, which enable minimally invasive implantation while ensuring strong tissue fixation and reduced complications.
Percutaneous implantation
- Prostate
- Lung
- Abdominal organs such as liver, pancreas, kidney, adrenal gland and metastases in various places
- Breast
- Cervix and other gynecologic organs
- Bladder wall
- Head & neck applications such as tonsil, nodules, base of tongue and close to the larynx
Endoscopic implantation
Placement of Gold Anchor through endoscope is possible by using Gold Anchor Introducer. The Gold Anchor Introducer is delivered pre-loaded with the Gold Anchor marker inside. Then can Gold Anchor also be placed in:
- Rectal
- Esophageal
- Pancreatic and central lung tumors
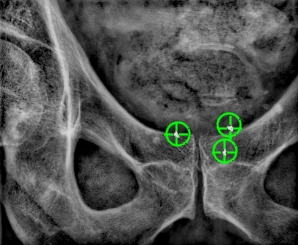
Prostate
Fiducial markers are often used to guide external beam radiotherapy for prostate to provide target coverage while protecting nearby sensitive organs. The fiducial markers can be used for the treatment planning, daily patient setup and for intrafraction motion management during treatment. Using fiducial markers for prostate radiotherapy have proven to increase accuracy, reduce side effects and improve treatment outcome.
Gold Anchorʼs industry leading thin needles and unique anchoring marker design makes it possible to proceed with CT/MR for dose planning on the same day as implantation. The Gold Anchor markers are also visible on MRI due to unique and patented material. Gold Anchor can also be tracked in real-time during treatment with kV-imaging.
Usage in prostateBreast
Gold Anchor can be used for both radiotherapy and surgery of breast cancer. For surgery of breast cancer patients, it is common to place a marker or clip at the time of biopsy to guide the surgeon for the excision. During surgery the marker is removed.
Radiation therapy is commonly used in the treatment of breast cancer for example for adjuvant therapy after surgery. Boost treatment is becoming more and more common as well as the delineation of the target area on MRI. Gold Anchor markers provide strong tissue attachment in the tumor bed and provide good visibility both on kV and MR images.
Biopsy marking Radiation therapyLung
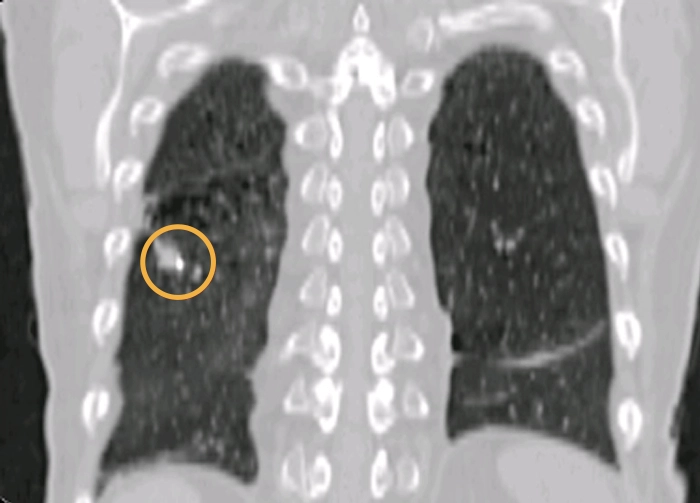
Lung tumors can often be visualized with cone-beam CT but there are cases that can benefit from using fiducial markers, e.g. when there is atelectasis or when the tumor edges as blurry. Gold Anchorʼs industry leading thin needles drastically reduces the risk of transthoracic implantation. With the Gold Anchor Introducer the markers can also be placed using bronchoscopy.
Lung radiotherapy Lung surgeryAbdominal
Gold Anchor is suitable for percutaneous implantation in most soft tissue organs, e.g. liver, pancreas, kidney, adrenal gland, breast, oligomets in abdomen and inguinal metastases. Gold Anchor is available in the same type of ultrathin needles that have been used for over 60 years for fine needle aspiration cytology (FNAC) with no to very little harm.
Usage in abdominalGynecologic
The cervix is prone to movement. Fiducial markers are therefore useful to guide both external-beam and internal radiotherapy (brachy). However, traditional markers tend to migrate and fall out of the vaginal wall and cervix while Gold Anchors expand outside the needle and anchor in the tissue.
Usage in gynecologicEndoscopic
Placement of Gold Anchor through endoscope in central lung, esophagus, pancreas, and rectal tumors is possible by using Gold Anchor Introducer. Gold Anchor Introducer is delivered pre-loaded with the Gold Anchor marker inside. The Gold Anchor Introducer is not available for sale in in all Gold Anchor markets.
Usage in endoscopic